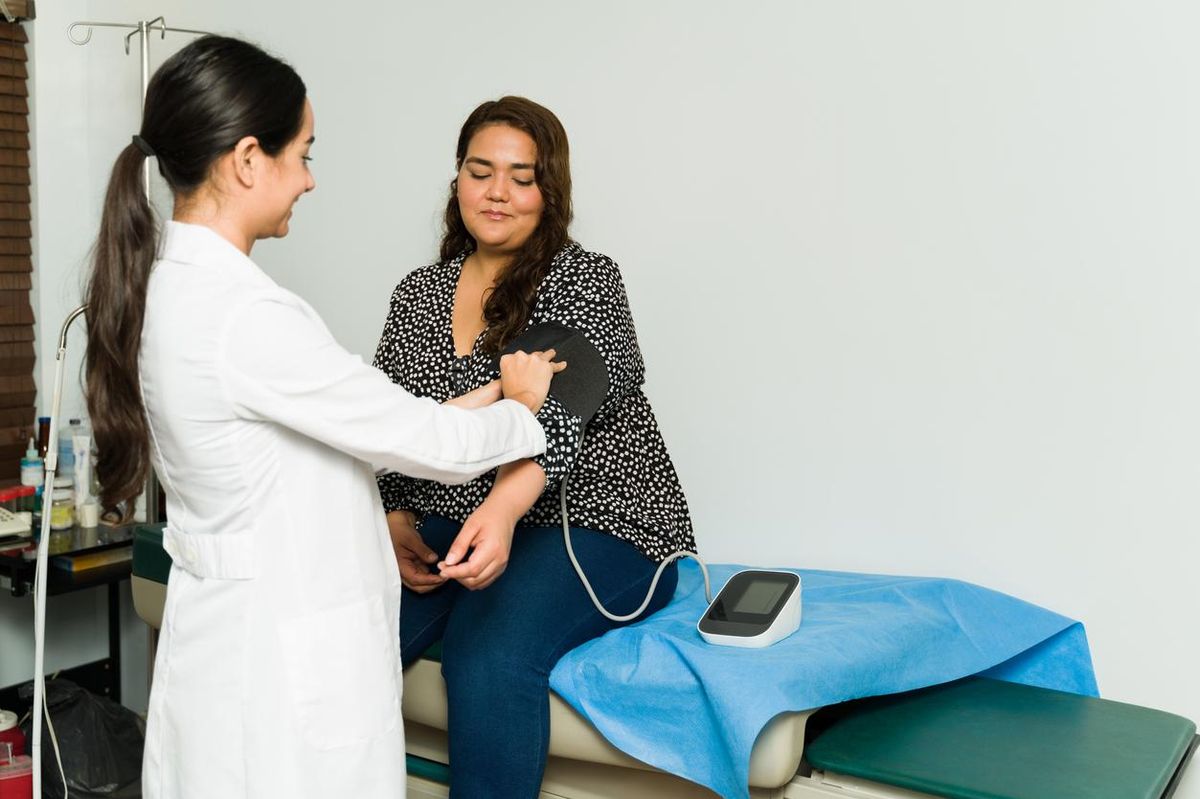
If you’re a woman between the ages of 40 and 65, you’ve probably experienced any number of stressors, including financial, social, physical, mental health and emotional challenges.
Women in midlife carry numerous responsibilities — for jobs and careers, parents, children, and partners and friends. They may also be experiencing personal health issues while experiencing menopause, which occurs after 12 months have passed without a period. The transition to menopause, called perimenopause, often brings biological and psychological changes that can be disruptive, uncomfortable, unsettling or even embarrassing. Worse than experiencing negative effects of menopause, many women face them alone, uncomfortable and unable to share their experiences with friends, family members or even their healthcare providers (HCPs).
Women sometimes even perceive that their HCPs don’t feel comfortable discussing menopause, leaving many women without the information or treatment they need.
To support open dialogue about women’s health during midlife and identify what information women most need about their health, HealthyWomen brought together a group of HCPs and advocates to discuss the barriers women face in accessing information, resources and treatments as they age.
Roundtable participants identified several specific health issues that particularly affect women in midlife, including:
- Arthritis
- Bladder issues
- Bone issues
- Brain issues
- Diabetes
- Heart issues
- Mental health issues
- Sexual health issues
The roundtable discussion also focused heavily on menopause, perhaps the most universal experience among midlife women. That said, no two women experience menopause exactly the same way. Many people think of hot flashes as the main symptom of menopause, but women experience a wide range of menopause symptoms, including changes to their sex drive, hair, skin, mood, sleep and cognition, and urinary health issues, such as increased frequency or urgency of urination, infections, prolapse and bladder control challenges.
As one roundtable participant put it, “We all get our own ticket to the hormonal roller-coaster ride.”
During midlife, it’s not just physical and emotional symptoms that can interfere with women feeling their best. Communication challenges between women and their HCPs can also serve as barriers to women getting the care they need and deserve.
Too often, women report not feeling heard, understood or taken seriously by HCPs. As a result, many women lose trust in their providers and in the healthcare system overall.
Adding to the confusion among some women in midlife is that guidance on certain treatments, such as hormone therapy (HT) — previously called hormone replacement therapy or HRT — has changed over several decades. The changing clinical guidance has led some women and even some HCPs to be less certain about the best way to treat perimenopause symptoms. To find relief, some women turn to alternate remedies, not all of which are grounded in scientific evidence.
Not all HCPs take these remedies seriously and, in turn, women can feel that their HCP doesn’t take their symptoms seriously or offer viable treatment options.
Even when it may be clear what women can and should do to improve or maintain their health, not all women have the same access to healthcare. Women of color, lower-income women and women in other marginalized groups often experience bias that gets in the way of getting the information and treatment they need. Roundtable participants discussed the need for HCPs to have more training and greater sensitivity to unintended or implicit bias.
“Cultural humility means you don’t assume you know anything about any patient, and you don’t take the way she’s dressed or the color of her skin or anything else and just assume you know something,” one participant said.
Experts also agreed that all women should be able to get reliable, understandable information in a manner that meets them where they are. Participants stressed the importance of women feeling empowered and equipped to discuss their own health and healthcare, and to understand what their HCP tells them.
For too many women, midlife can be a stressful, lonely time.
As their health and healthcare needs change, many don’t know where to turn for trusted information or guidance. HCPs often lack the time, training or comfort to openly discuss menopause, related symptoms and possible treatments. Employers may be able to play a role by designing workplace policies to accommodate women’s needs during perimenopause, just as many employers have done for pregnant and breastfeeding workers. Through accommodations, employers can also help reduce stigma that still surrounds menopause.
The future may be bright, though, according to participants.
They discussed that norms may be changing and that younger women are more open and willing to discuss previously taboo topics. With more open discussion earlier in life, younger women may help demystify menopause and be better prepared to navigate their own journey.
Original Article